The Turning Point in Healthcare
Healthcare is undergoing a profound metamorphosis. Not incremental. Not optional. Foundational. What once evolved slowly over decades is now accelerating at a pace that is impossible to ignore. The rules are changing, and more importantly, the expectations are changing with them.
For decades, healthcare systems have been designed to respond—to symptoms, to emergencies, to crises. A patient feels unwell, seeks care, receives treatment, and exits the system until the next issue arises. It is a cycle built on reaction. Functional, yes. But increasingly inadequate in a world driven by data, intelligence, and immediacy.
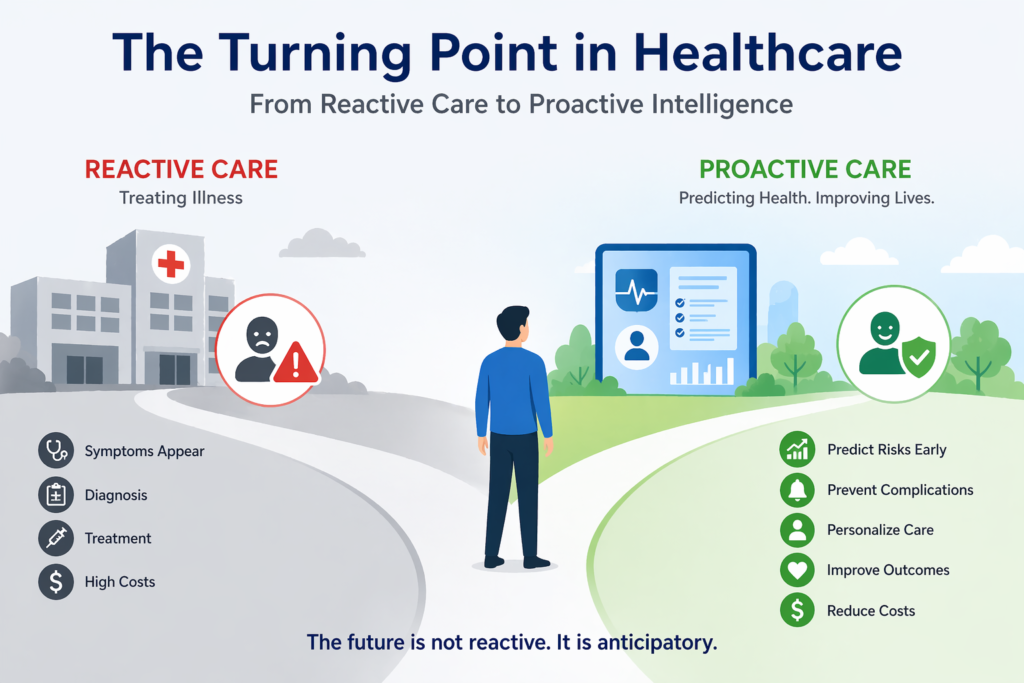
Today, a different expectation is emerging. One that prioritizes foresight over reaction. Precision over approximation. Continuity over episodic care. Patients are no longer satisfied with being treated only when something goes wrong. They expect healthcare systems to anticipate risks, guide outcomes, and remain engaged throughout their journey.
At the center of this transformation is the convergence of artificial intelligence and CRM platforms—particularly solutions like Salesforce Health Cloud. These technologies are not just enhancing existing processes; they are redefining them. By unifying patient data, enabling real-time insights, and embedding predictive intelligence into workflows, they are turning healthcare into a proactive, continuously evolving ecosystem.
“The best way to predict the future is to create it.” — Peter Drucker
Healthcare is finally taking that advice seriously. And in doing so, it is shifting from a system that reacts to illness to one that actively works to prevent it.
What’s Changing at a Glance
The transformation can be understood through a few fundamental shifts:
- Care is shifting from episodic → continuous
Healthcare is no longer limited to appointments and hospital visits. It is becoming an ongoing, always-on engagement model. - Data is shifting from fragmented → unified
Disconnected systems are being replaced by integrated platforms that provide a complete view of the patient. - Decisions are shifting from reactive → predictive
Instead of responding to symptoms, healthcare providers can now anticipate risks using AI-driven insights. - Systems are shifting from passive → intelligent
Technology is no longer just storing information—it is actively guiding decisions and triggering actions.
This is not a subtle evolution. It is a structural reinvention of how healthcare operates, how providers deliver care, and how patients experience it.
And for organizations that recognize this turning point, the opportunity is not just to improve care—but to redefine it entirely.
Table of Contents
- The Turning Point in Healthcare
- Understanding Reactive Care: The Traditional Model
- The Limitations of Treat-After-Diagnosis Systems
- Rising Patient Expectations in the Digital Age
- What Is Proactive Care? A Paradigm Shift
- 6. The Role of Data in Modern Healthcare
- Breaking Down Data Silos in Healthcare Systems
- Enter AI in Healthcare: More Than Just Automation
- How Predictive Analytics Is Changing Clinical Decisions
- The Power of CRM in Healthcare Transformation
- What Makes Salesforce Health Cloud a Game-Changer
- Real-Time Patient Insights: From Records to Intelligence
- The Role of Salesforce Einstein in Predictive Care
- Personalized Patient Journeys at Scale
- Automating Preventive Care Workflows
- Reducing Hospital Readmissions with Smart Systems
- Enhancing Care Coordination Across Teams
- The Business Impact of Proactive Healthcare
- Compliance, Security, and Trust in AI-Driven Systems
- Challenges in Adopting Proactive Care Models
- How to Successfully Transition from Reactive to Proactive Care
- Real-World Use Cases of AI + CRM in Healthcare
- The Future of Healthcare: Autonomous, Intelligent, Predictive
- Why Healthcare Organizations Must Act Now
- Conclusion: The New Standard of Care
- How CloudVandana Enables Proactive Healthcare Transformation
- Frequently Asked Questions (FAQs)
- 1. What is proactive healthcare?
- 2. How is proactive care different from reactive care?
- 3. What role does AI play in proactive healthcare?
- 4. How does CRM help in healthcare transformation?
- 5. What is Salesforce Health Cloud used for?
- 6. Can proactive healthcare reduce hospital readmissions?
- 7. How does predictive analytics improve patient outcomes?
- 8. Is proactive healthcare only for large hospitals?
- 9. How secure is patient data in AI-driven healthcare systems?
- 10. What challenges do organizations face when adopting proactive care?
- 11. How long does it take to implement Salesforce Health Cloud?
- 12. How can CloudVandana help healthcare organizations?
- YOU MIGHT ALSO LIKE
Understanding Reactive Care: The Traditional Model
Reactive care has long been the backbone of healthcare systems across the globe. It is familiar, structured, and deeply embedded in how care is delivered today. At its core, the model follows a straightforward sequence:
- A patient experiences symptoms
- The patient seeks medical attention
- A diagnosis is made
- Treatment is administered
This approach has undeniably saved millions of lives. It has formed the foundation of modern medicine and continues to play a critical role in acute and emergency care scenarios. However, its simplicity is also its limitation.
The fundamental issue with reactive care is not what it does—it is when it does it.
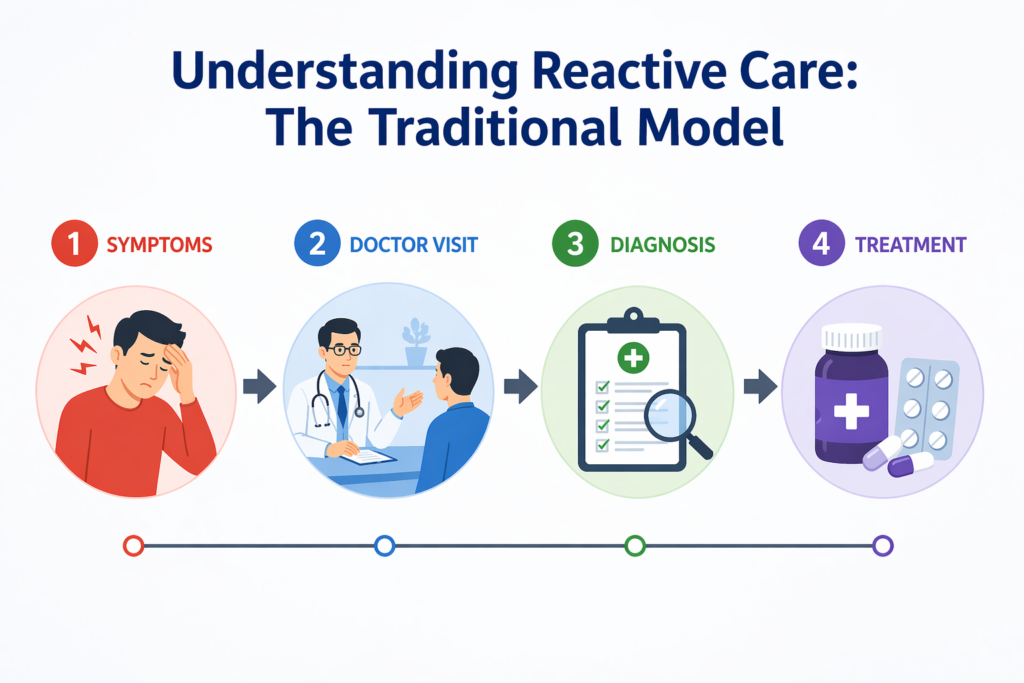
By the time a patient enters the system, the condition has already developed, and in many cases, progressed. The model is designed to respond after the problem has surfaced, not before. And in healthcare, timing is everything.
Key Characteristics of Reactive Care
A closer look at this model reveals several inherent patterns:
- Symptom-driven decision making
Care is initiated only when visible or felt symptoms appear. Silent conditions or early-stage risks often go undetected. - Limited visibility into patient history
Disconnected systems and fragmented data mean providers rarely have a complete, real-time view of the patient’s health journey. - Minimal preventive intervention
Preventive care exists, but it is not deeply embedded into workflows. It relies heavily on scheduled check-ups rather than continuous monitoring. - High dependency on patient-initiated visits
The responsibility to seek care lies primarily with the patient. If they delay, ignore symptoms, or lack awareness, intervention is delayed as well.
Why This Model Falls Short Today
In a world driven by data and real-time intelligence, reactive care feels increasingly outdated. It is inherently defensive—built to respond rather than anticipate.
Consider chronic conditions like diabetes or heart disease. These do not appear overnight. They develop gradually, often with subtle warning signs. A reactive system overlooks these early signals, only stepping in when the condition demands attention.
This leads to:
- Higher treatment costs
- Increased hospital admissions
- Poorer patient outcomes
- Greater strain on healthcare systems
The model, while effective in critical situations, lacks the capability to prevent those situations from occurring in the first place.
And that is the core problem.
Reactive care does not fail because it is ineffective. It fails because it is incomplete.
It addresses the consequence, not the cause.
The Limitations of Treat-After-Diagnosis Systems
The inefficiencies of reactive care are no longer subtle. They are visible in rising costs, overburdened systems, and—most critically—missed opportunities to intervene early. What once worked in a less connected world is now struggling to keep pace with the complexity of modern healthcare.
At its core, the limitation is simple: the system waits. And in healthcare, waiting often comes at a high price.
Key Limitations of Reactive Care
- Delayed diagnosis leads to advanced-stage diseases
Many conditions—especially chronic and lifestyle-related illnesses—develop gradually. Without continuous monitoring or early detection mechanisms, they remain unnoticed until symptoms become severe. By then, treatment becomes more complex, more expensive, and less effective. - Repetitive hospital visits increase operational strain
When underlying issues are not addressed proactively, patients tend to cycle through the system repeatedly. Emergency visits, follow-ups, and readmissions become common, placing immense pressure on healthcare infrastructure and staff. - Lack of continuity leads to poor patient outcomes
Reactive care is episodic. Each visit is treated as an isolated event rather than part of a continuous journey. This lack of longitudinal visibility prevents providers from understanding patterns, leading to fragmented and often suboptimal care decisions. - Fragmented records result in incomplete clinical decisions
Patient data is often scattered across multiple systems—EHRs, lab reports, imaging platforms, and communication tools. Without a unified view, clinicians are forced to make decisions based on partial information, increasing the risk of errors and inefficiencies.
“Healthcare systems are not short on data. They are short on connected data.”
This distinction is critical. Data exists in abundance, but its true value remains locked behind silos.
A Real-World Scenario
Consider a patient managing diabetes.
They miss a few routine check-ups. No system flags the absence. No automated reminder is triggered. No care coordinator reaches out. Over time, blood sugar levels fluctuate unnoticed. Complications begin to develop silently.
Months later, the patient is admitted with severe complications—something that could have been prevented with timely intervention.
This is not a rare occurrence. It is a systemic pattern.
The Core Problem: Lack of Anticipation
Reactive care does not fail because healthcare professionals lack expertise or commitment. It fails because the system itself is not designed to anticipate risk.
It operates in hindsight, not foresight.
- It treats outcomes instead of predicting them
- It responds to events instead of preventing them
- It reacts to symptoms instead of monitoring signals
In a data-rich, AI-enabled world, this approach is no longer sustainable.
The future of healthcare demands more than reaction. It demands anticipation.
Rising Patient Expectations in the Digital Age
Patients today are no longer passive recipients of care. They are informed, connected, and increasingly discerning about the experiences they receive. Access to information, digital tools, and on-demand services has fundamentally reshaped how individuals perceive healthcare.
What was once accepted as “normal” is now being questioned.
Why should booking a medical appointment be harder than ordering food?
Why should accessing health records be slower than checking a bank balance?
Why should communication with providers feel fragmented in a world of instant connectivity?
These comparisons are no longer hypothetical—they are shaping expectations in real time.
Influenced by seamless digital experiences across industries like retail, banking, and travel, patients now expect healthcare systems to operate with the same level of efficiency, personalization, and responsiveness. And increasingly, they are choosing providers who can deliver on those expectations.
What Modern Patients Expect
- Real-time communication
Patients expect instant updates—appointment confirmations, test results, reminders, and follow-ups—without delays or manual intervention. Waiting days for information is no longer acceptable. - Personalized treatment plans
One-size-fits-all care models are losing relevance. Patients want care tailored to their medical history, lifestyle, and preferences—not generic recommendations. - Seamless digital interactions
From booking appointments to accessing records, every touchpoint is expected to be intuitive, connected, and frictionless. Multiple logins, repeated form-filling, and disconnected systems create frustration. - Continuous monitoring and follow-ups
Care is no longer viewed as a one-time interaction. Patients expect ongoing engagement—whether through remote monitoring, automated check-ins, or proactive outreach from providers.
The Experience Gap in Healthcare
Despite these expectations, many healthcare systems still operate on legacy infrastructure—fragmented, slow, and reactive. This creates a widening gap between what patients expect and what they experience.
A disconnected system cannot deliver a connected experience.
When data is siloed, communication breaks down. When workflows are manual, delays become inevitable. When insights are missing, personalization becomes impossible.
A Shift Beyond Treatment
Healthcare is no longer defined solely by clinical outcomes. It is increasingly measured by experience.
- How quickly was the patient attended to?
- How well was their history understood?
- How seamless was their journey across departments?
- How proactively was their care managed?
These factors now influence trust, satisfaction, and long-term loyalty.
Healthcare is no longer just about treatment.
It is about experience.
What Is Proactive Care? A Paradigm Shift
Proactive care represents a decisive break from traditional healthcare models. It does not wait for illness to surface before taking action. Instead, it seeks to understand, anticipate, and mitigate risk long before it evolves into a clinical issue.
Where reactive care is event-driven, proactive care is intelligence-driven.
It operates on a simple but powerful premise: the earlier a risk is identified, the better the outcome. This shift fundamentally changes how healthcare is delivered—not as a series of isolated interactions, but as a continuous, data-informed journey.
Rather than responding to symptoms, proactive care focuses on signals. Subtle changes in behavior, patterns in clinical data, and early indicators that might otherwise go unnoticed are brought to the forefront. The goal is not just to treat illness, but to prevent it from occurring in the first place.
How Proactive Care Redefines the Model
- Instead of waiting for symptoms → it identifies risk patterns early
- Instead of isolated treatments → it enables continuous engagement
- Instead of episodic care → it builds long-term patient relationships
- Instead of reactive decisions → it drives predictive interventions
This transformation is not incremental. It is structural.
Core Principles of Proactive Care
- Early risk detection
Advanced analytics and AI models analyze historical and real-time data to flag potential health risks before they escalate. This enables timely interventions and reduces the likelihood of severe complications. - Continuous patient monitoring
Through connected systems and wearable technologies, patient health is tracked beyond clinical settings. Providers gain ongoing visibility into vital metrics, enabling them to act when deviations occur. - Preventive interventions
Instead of waiting for conditions to worsen, proactive systems trigger early actions—routine check-ups, medication adjustments, lifestyle recommendations, and targeted outreach. - Personalized care journeys
Each patient’s journey is tailored based on their medical history, behavior patterns, and risk profile. Care becomes individualized, not standardized.
“The greatest medicine of all is teaching people how not to need it.” — Hippocrates
Proactive care embodies this philosophy.
The Role of Technology in Enabling Proactive Care
Achieving this level of intelligence and coordination is not possible through manual processes or disconnected systems. It requires a unified digital foundation—one that brings together data, workflows, and insights in real time.
This is where platforms like Salesforce Health Cloud play a critical role.
By centralizing patient information, integrating with multiple data sources, and embedding AI-driven intelligence into workflows, Health Cloud transforms how care is delivered. It enables healthcare providers to move beyond reactive decision-making and adopt a proactive, patient-centric approach at scale.
The result is a system that does not just respond to illness—but actively works to prevent it.
And that is the future of healthcare.
6. The Role of Data in Modern Healthcare
Data is the lifeblood of proactive healthcare. It fuels every insight, informs every decision, and underpins every meaningful intervention. In a system that aims to anticipate rather than react, data is not just important—it is indispensable.
Every appointment, diagnosis, prescription, and patient interaction generates a trail of information. Individually, these data points may seem routine. Collectively, they form a powerful narrative about a patient’s health journey.
But there is a critical distinction.
More data does not automatically mean better care.
Without structure, context, and intelligence, data becomes noise—overwhelming, fragmented, and difficult to interpret. Healthcare providers are often inundated with information but lack the tools to convert it into actionable insights.
Understanding the Different Types of Healthcare Data
To fully appreciate the role of data, it is important to recognize its diversity:
- Clinical data (EHRs, lab reports)
This forms the backbone of patient health information—diagnoses, test results, medical history, treatment plans. It provides a clinical snapshot but often lacks real-time updates. - Behavioral data (lifestyle, adherence)
Insights into how patients live—their habits, routines, medication adherence, and lifestyle choices. This data is crucial for managing chronic conditions and predicting long-term outcomes. - Interaction data (appointments, communication)
Every touchpoint between patient and provider—appointments, follow-ups, calls, emails. This data reveals engagement levels and potential gaps in care. - Device data (wearables, IoT health monitors)
Continuous streams of real-time data from smart devices—heart rate, activity levels, sleep patterns, glucose monitoring. This is where proactive care gains its edge.
From Data Collection to Data Activation
Most healthcare systems are already rich in data. The real challenge lies elsewhere.
It is not about collecting more data.
It is about activating the data that already exists.
Activation means:
- Connecting data across systems
- Analyzing it in real time
- Translating it into actionable insights
- Triggering timely interventions
This is where modern platforms like Salesforce Health Cloud play a transformative role. By unifying disparate data sources into a single, comprehensive view, they enable healthcare providers to move from passive data storage to active data utilization.
Why Data Activation Matters
When data is properly activated:
- Risks are identified earlier
- Decisions are more informed
- Care becomes personalized
- Outcomes improve significantly
A patient’s story is no longer scattered across systems. It becomes a continuous, evolving narrative—one that healthcare providers can understand, anticipate, and act upon.
In the context of proactive care, data is not just a resource.
It is a strategic advantage.
Breaking Down Data Silos in Healthcare Systems
Healthcare systems are notoriously fragmented. Not because of a lack of technology, but because of how that technology has evolved—independently, in silos, and often without interoperability as a priority.
Different departments operate on different systems. Each optimized for its own function, yet disconnected from the larger ecosystem. The result? Data exists everywhere, but insight exists nowhere.
A patient’s journey, instead of being a single, continuous narrative, is scattered across multiple touchpoints—each holding a piece of the truth, but none capturing the full picture.
Where Data Silos Typically Exist
- Electronic Health Records (EHR)
Store clinical history, diagnoses, and treatment plans—but often remain isolated within specific providers or departments. - Billing systems
Capture financial transactions and insurance details, yet rarely integrate seamlessly with clinical data for a holistic view. - Lab systems
Generate critical diagnostic information, but may not sync in real time with primary care or specialist platforms. - Communication tools
Emails, call logs, and appointment systems track patient interactions but often exist outside core clinical systems.
Each of these systems serves a purpose. But when they operate in isolation, they create blind spots.
The Real Impact of Fragmentation
Data silos are not just a technical inconvenience. They have direct consequences on care quality and operational efficiency:
- Redundant tests
Without access to complete records, providers may repeat diagnostic tests, increasing costs and delaying treatment. - Delayed decisions
Critical information may not be available at the right time, forcing clinicians to wait—or worse, make decisions with incomplete data. - Poor care coordination
Specialists, primary care providers, and support staff may operate without full visibility, leading to misalignment and gaps in care.
“Silos don’t just store data. They store inefficiency.”
Why Breaking Silos Is Essential for Proactive Care
Proactive care depends on continuity. Continuity depends on visibility. And visibility depends on integration.
Without a unified view of patient data:
- Early warning signs are missed
- Patterns go undetected
- Preventive interventions are delayed
In other words, proactive care becomes impossible.
The Role of CRM in Unifying Healthcare Data
This is where CRM platforms fundamentally change the equation.
Solutions like Salesforce Health Cloud eliminate silos by creating a centralized, unified data layer. Instead of replacing existing systems, they integrate with them—bringing all relevant data into a single, accessible interface.
What this enables:
- A 360-degree view of the patient
- Real-time access to clinical and non-clinical data
- Seamless collaboration across departments
- Faster, more informed decision-making
From Fragmentation to Fluidity
When silos are broken, healthcare shifts from fragmented to fluid.
Information flows freely. Teams collaborate effectively. Patients experience continuity instead of confusion.
And most importantly, providers gain the clarity they need to move from reacting to problems… to preventing them altogether.
Enter AI in Healthcare: More Than Just Automation
Artificial intelligence is redefining healthcare intelligence.
It goes beyond automation. It interprets data, identifies patterns, and predicts outcomes.
AI capabilities in healthcare:
- Pattern recognition
- Risk prediction
- Decision support
- Workflow optimization
“AI will not replace doctors. But doctors who use AI will replace those who don’t.”
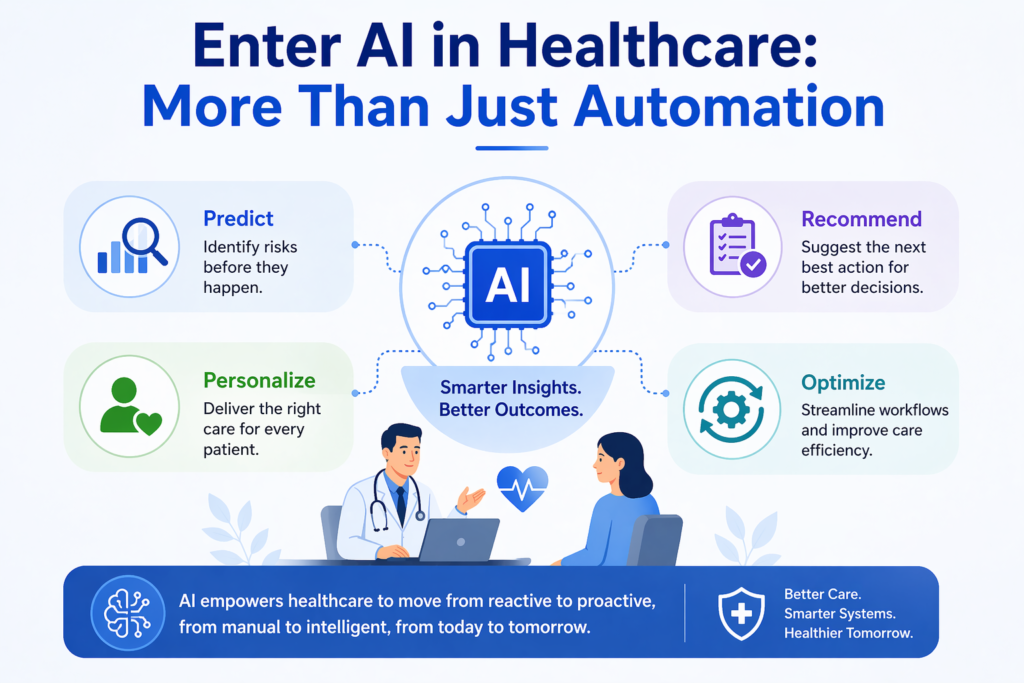
AI enhances human decision-making rather than replacing it.
How Predictive Analytics Is Changing Clinical Decisions
Predictive analytics transforms hindsight into foresight. It shifts the clinical lens from what has already happened to what is likely to happen next. In a system historically driven by retrospective analysis, this capability is nothing short of revolutionary.
By analyzing vast volumes of historical data alongside real-time inputs, predictive models can detect patterns that are invisible to the human eye. Subtle variations in vitals, behavioral trends, and clinical histories are interpreted not as isolated data points—but as signals of potential risk.
The result is a fundamental shift in decision-making.
Clinicians are no longer reacting to symptoms alone. They are anticipating outcomes.
How Predictive Analytics Works in Practice
At its core, predictive analytics combines:
- Historical patient data
- Real-time health indicators
- Machine learning algorithms
- Risk scoring models
These elements work together to generate insights that guide clinical action—often before a condition becomes critical.
Key Applications in Healthcare
- Predicting patient deterioration
Continuous monitoring of vital signs allows systems to detect early warning signals—minute changes that may indicate declining health. Alerts can be triggered before the situation escalates. - Identifying high-risk chronic patients
Patients with conditions like diabetes, heart disease, or hypertension can be continuously assessed for risk levels. This enables targeted interventions and better long-term management. - Forecasting readmission probabilities
By analyzing discharge data, treatment history, and behavioral patterns, systems can predict which patients are more likely to be readmitted—and initiate preventive follow-ups. - Optimizing treatment pathways
Predictive models can recommend the most effective treatment plans based on similar patient profiles, improving both outcomes and efficiency.
Case Insight: Early Intervention in Action
A leading hospital system implemented predictive analytics to monitor patient vitals in real time. By identifying early warning signs—subtle fluctuations in heart rate, oxygen levels, and other indicators—the system flagged patients at risk of deterioration.
The outcome was significant.
- ICU admissions were reduced
- Early interventions increased
- Patient outcomes improved
What once required visible symptoms now relied on invisible signals.
From Data to Life-Saving Decisions
This is where predictive analytics proves its true value.
It is not just about improving operational efficiency or reducing costs—although it does both. It is about enabling timely interventions that can prevent complications, reduce suffering, and, in many cases, save lives.
“In healthcare, the difference between early and late is often the difference between manageable and critical.”
Predictive analytics ensures that healthcare providers are not just informed—but prepared.
And in a proactive care model, that preparation makes all the difference.
The Power of CRM in Healthcare Transformation
CRM systems are the connective tissue of proactive healthcare. They do not merely store information—they orchestrate it. They bring together disparate data points, align stakeholders, and create a continuous, intelligent flow of information across the entire care journey.
In a fragmented ecosystem, CRM acts as the unifying layer. In a proactive model, it becomes the command center.
Where traditional healthcare systems focus on records, CRM platforms focus on relationships. That distinction changes everything.
From Data Silos to a Unified Patient View
At the heart of proactive care lies a simple requirement: visibility.
Healthcare providers need to see the full picture—not just isolated snapshots. CRM systems make this possible by aggregating data from multiple sources into a single, comprehensive patient profile.
Solutions like Salesforce Health Cloud are purpose-built for this transformation.
They unify:
- Clinical records
- Appointment histories
- Communication logs
- Behavioral insights
- Care plans and outcomes
The result is a 360-degree patient view—a living, evolving profile that informs every decision.
Key CRM Capabilities Driving Proactive Care
- Centralized patient profiles
Every piece of patient data is accessible in one place. No switching between systems. No missing context. This ensures that every provider works with the same, complete information. - Real-time communication tracking
Every interaction—calls, messages, follow-ups—is logged and visible. This eliminates communication gaps and ensures patients never feel overlooked. - Workflow automation
Routine processes such as appointment reminders, follow-ups, and care plan updates are automated. This reduces manual effort while improving consistency and responsiveness. - Care coordination across teams
Multiple stakeholders—doctors, nurses, specialists, administrators—can collaborate seamlessly. Everyone is aligned. Everyone is informed.
From Systems of Record to Systems of Engagement
Traditional healthcare platforms are designed to record events. CRM platforms are designed to drive engagement.
This shift is subtle but powerful.
- Instead of documenting past interactions → CRM enables future actions
- Instead of storing static data → CRM activates dynamic workflows
- Instead of isolated departments → CRM connects entire care ecosystems
“The goal is not to collect more data. The goal is to create better decisions.”
A Practical Scenario
Consider a patient recently discharged after cardiac treatment.
In a traditional system:
- Discharge happens
- Follow-up depends on manual scheduling
- Patient engagement is inconsistent
In a CRM-driven system:
- Automated follow-ups are triggered
- Care coordinators receive alerts for high-risk patients
- Patients receive reminders and personalized guidance
- Providers track adherence and intervene early if needed
The difference is not just operational. It is clinical.
The Strategic Impact of CRM in Healthcare
When CRM is fully integrated into healthcare workflows:
- Patient engagement becomes continuous
- Risks are identified earlier
- Care becomes personalized at scale
- Outcomes improve significantly
CRM transforms healthcare from a system of records into a system of relationships.
And in a proactive care model, relationships are everything.
Because the future of healthcare is not just about treating patients.
It is about understanding them, engaging them, and guiding them—before treatment is ever needed.
What Makes Salesforce Health Cloud a Game-Changer
Salesforce Health Cloud is designed specifically for healthcare ecosystems.
It provides a comprehensive, 360-degree view of patients.
Key capabilities:
- Unified patient profiles
- Care plan management
- Integration with EHR systems
- Real-time patient insights
Impact:
- Faster decision-making
- Improved patient engagement
- Reduced operational inefficiencies
Real-Time Patient Insights: From Records to Intelligence
Traditional systems store data. Modern systems activate it.
Real-time insights allow healthcare providers to act immediately.
Examples:
- Alerts for missed medications
- Notifications for abnormal vitals
- Automated follow-up reminders
Information becomes actionable. Instantly.
The Role of Salesforce Einstein in Predictive Care
If CRM is the connective tissue of proactive healthcare, intelligence is what brings it to life.
This is where Salesforce Einstein plays a pivotal role.
It does not just process data—it interprets it. It does not just present information—it guides decisions. By embedding artificial intelligence directly into CRM workflows, Einstein transforms static systems into adaptive, learning-driven environments.
In a proactive care model, this shift is critical.
From Data Analysis to Intelligent Action
Traditional systems rely on human interpretation. Clinicians review reports, analyze trends, and make decisions based on experience and available information.
Einstein accelerates and augments this process.
It continuously analyzes:
- Historical patient data
- Real-time health indicators
- Behavioral patterns
- Interaction history
And converts these into actionable insights—instantly.
Core Capabilities of Salesforce Einstein in Healthcare
- Predictive scoring for patient risk
Einstein evaluates patient data to assign risk scores—identifying individuals who are more likely to experience complications, deterioration, or readmission. This allows providers to prioritize care where it is needed most. - Next-best action recommendations
Instead of leaving decisions entirely manual, Einstein suggests the most effective next step—whether it’s scheduling a follow-up, adjusting treatment, or initiating preventive outreach. - Automated insights generation
Patterns that would typically go unnoticed are surfaced automatically. Clinicians are alerted to anomalies, trends, and opportunities for intervention without needing to manually search for them.
A Shift in Clinical Decision-Making
This is where the transformation becomes tangible.
- Decisions are no longer based solely on current symptoms
- Insights are no longer delayed or manually derived
- Actions are no longer reactive
Instead, healthcare providers operate with a forward-looking perspective—supported by intelligence that is continuously learning and improving.
“In complex systems, the best decisions are not just informed—they are assisted.”
Practical Impact in a Healthcare Setting
Consider a patient with a history of hypertension.
Without AI:
- Monitoring depends on periodic visits
- Risk escalation may go unnoticed between check-ups
With Einstein:
- Patient data is continuously analyzed
- Risk scores are updated dynamically
- Alerts are triggered when thresholds are crossed
- Providers receive recommendations for intervention
What changes is not just speed—but accuracy and consistency.
From CRM to Decision Engine
When intelligence is embedded into CRM, the system evolves.
- From storing data → to understanding it
- From tracking interactions → to predicting outcomes
- From supporting workflows → to driving them
CRM becomes more than a platform. It becomes a decision-making engine.
And in healthcare, where timing and precision are critical, that evolution is not just beneficial.
It is essential.
Personalized Patient Journeys at Scale
Healthcare is moving toward personalization.
No two patients are identical. Their care journeys should not be either.
Personalization enables:
- Tailored communication
- Customized care plans
- Targeted interventions
This improves both outcomes and patient satisfaction.
Automating Preventive Care Workflows
Preventive care requires consistency. Automation ensures it.
Using tools like Salesforce Flow, healthcare providers can:
- Automate appointment reminders
- Trigger follow-ups based on conditions
- Ensure medication adherence tracking
Manual processes are replaced by intelligent workflows.
Reducing Hospital Readmissions with Smart Systems
Hospital readmissions remain one of the most persistent and expensive challenges in healthcare. They strain already stretched resources, inflate operational costs, and often signal gaps in post-treatment care.
More importantly, many readmissions are preventable.
The issue is not always the quality of treatment delivered during hospitalization—it is what happens after discharge. Without structured follow-up, continuous monitoring, and timely intervention, patients can quickly relapse or develop complications that require readmission.
This is where predictive systems change the equation.
From Reactive Readmissions to Proactive Prevention
Traditional models treat readmissions as outcomes to manage. Proactive systems treat them as risks to prevent.
By leveraging platforms like Salesforce Health Cloud combined with AI capabilities such as Salesforce Einstein, healthcare providers can identify at-risk patients before complications arise.
These systems analyze:
- Discharge summaries
- Patient history and comorbidities
- Medication adherence patterns
- Social and behavioral factors
- Real-time recovery indicators
The result is a dynamic risk profile that evolves as the patient recovers.
Key Strategies to Reduce Readmissions
- Post-discharge monitoring
Patients are continuously monitored after leaving the hospital. Vital signs, symptoms, and behavioral patterns are tracked through connected systems and devices. Any deviation triggers immediate attention. - Automated follow-ups
Instead of relying on manual outreach, systems automatically schedule and initiate follow-ups—calls, messages, or appointments—ensuring consistent engagement during the critical recovery period. - Personalized care plans
Recovery is not one-size-fits-all. Each patient receives tailored care plans based on their condition, history, and risk level. This improves adherence and reduces the likelihood of complications.
Case Study: Turning Insight into Impact
A healthcare provider implemented predictive CRM systems to track patient recovery post-discharge. By combining unified patient data with AI-driven risk scoring, they were able to identify individuals most likely to be readmitted.
Targeted interventions were then applied:
- High-risk patients received more frequent follow-ups
- Automated alerts ensured no patient was overlooked
- Care teams were notified of early warning signs
The outcome was measurable and significant:
- 25% reduction in hospital readmissions
- Improved patient recovery rates
- Reduced operational burden on hospital staff
Why This Matters
Readmissions are not just a cost issue. They are a care quality issue.
Each preventable readmission represents:
- A missed opportunity for early intervention
- A breakdown in continuity of care
- A negative patient experience
“The most effective care is the care that prevents the need for more care.”
Predictive systems ensure that recovery does not end at discharge. It becomes a monitored, guided journey—one where risks are anticipated, not discovered too late.
From Outcome Management to Outcome Prevention
This is the true shift.
- From reacting to readmissions → to preventing them
- From isolated discharge processes → to continuous recovery management
- From generic follow-ups → to personalized, data-driven care
And in a proactive healthcare model, that shift is not just valuable.
It is transformative.
Enhancing Care Coordination Across Teams
Healthcare delivery involves multiple stakeholders.
CRM platforms ensure everyone operates on the same data.
Benefits:
- Improved communication
- Reduced errors
- Faster decision-making
Care becomes collaborative rather than fragmented.
The Business Impact of Proactive Healthcare
Proactive care is often discussed in clinical terms—better outcomes, earlier interventions, improved patient safety. But its impact extends far beyond the clinical layer. It fundamentally reshapes the business dynamics of healthcare organizations.
When care becomes predictive and continuous, operations become smarter, costs become controlled, and patient relationships become stronger.
In other words, proactive care is not just a medical advantage. It is a strategic one.
From Cost Centers to Value Drivers
Traditional healthcare models tend to operate reactively—leading to inefficiencies, repeated interventions, and rising costs. Proactive care flips this equation.
By identifying risks early and preventing complications, healthcare organizations can shift from high-cost reactive treatments to lower-cost preventive strategies.
Key Business Benefits of Proactive Care
- Reduced operational costs
Preventing hospitalizations, minimizing readmissions, and avoiding redundant procedures significantly lowers overall costs. Early intervention is almost always more cost-effective than late-stage treatment. - Improved resource utilization
Hospitals and care teams can allocate resources more efficiently when they have visibility into patient risk levels. High-risk patients receive focused attention, while low-risk cases are managed through automated workflows. - Higher patient retention and loyalty
Patients who experience continuous, personalized care are more likely to stay engaged with a provider. Trust increases. Satisfaction improves. Long-term relationships are built. - Better revenue predictability
With structured care pathways and improved patient engagement, organizations gain more predictable patient flows and revenue streams. - Enhanced operational efficiency
Automation of routine tasks—appointments, follow-ups, care coordination—reduces administrative burden and allows healthcare professionals to focus on high-value activities.
Real-World Perspective
Healthcare providers that have adopted proactive care models often report:
- Fewer emergency admissions
- Lower cost per patient
- Improved staff productivity
- Higher patient satisfaction scores
These are not marginal gains. They are transformative improvements.
The Competitive Advantage
In an increasingly competitive healthcare landscape, differentiation is no longer based solely on clinical expertise. It is based on experience, efficiency, and outcomes.
Organizations that embrace proactive care:
- Deliver faster, more personalized services
- Build stronger patient relationships
- Operate with greater agility and insight
“Efficiency is doing things right. Effectiveness is doing the right things.” — Peter Drucker
Proactive care achieves both.
From Efficiency to Market Leadership
Healthcare organizations that invest in proactive models position themselves ahead of the curve.
They are not just reacting to industry changes. They are shaping them.
By leveraging platforms like Salesforce Health Cloud and embedding intelligence into operations, they create systems that are not only efficient—but adaptive, scalable, and future-ready.
The Bottom Line
Proactive care transforms healthcare from a reactive service model into a value-driven ecosystem.
- Costs decrease
- Outcomes improve
- Patients stay engaged
- Organizations grow stronger
And in a world where both clinical excellence and operational efficiency matter, that transformation is not optional.
It is essential.
Compliance, Security, and Trust in AI-Driven Systems
Data security in healthcare is not just a technical requirement. It is a foundational obligation. Every patient interaction, diagnosis, and record carries deeply sensitive information—and protecting that information is critical to maintaining both legal compliance and patient trust.
As healthcare systems evolve toward AI-driven, proactive models, the volume and velocity of data increase significantly. This creates a dual challenge: innovate faster while safeguarding more.
There is no room for compromise.
Why Security Is Non-Negotiable in Healthcare
Healthcare data is among the most sensitive categories of information. A breach does not just result in financial loss—it can erode patient confidence, damage institutional credibility, and lead to severe regulatory consequences.
Organizations must therefore strike a careful balance:
- Enable seamless data access for care delivery
- Restrict unauthorized exposure or misuse
- Maintain compliance across all processes
Innovation must happen within the boundaries of trust—not outside them.
Core Security Measures in Modern Healthcare Systems
To achieve this balance, robust security frameworks are essential. These typically include:
- Data encryption
Patient data is encrypted both at rest and in transit. This ensures that even if data is intercepted, it remains unreadable and protected from unauthorized access. - Access controls
Role-based access ensures that only authorized personnel can view or modify specific data. A nurse, a specialist, and an administrator each see only what is relevant to their responsibilities. - Audit trails
Every interaction with patient data is logged. Who accessed it, when, and what actions were taken. This creates accountability and enables rapid investigation in case of anomalies.
Compliance as a Continuous Process
Regulatory compliance in healthcare is not a one-time achievement—it is an ongoing commitment.
Frameworks such as HIPAA, GDPR, and regional data protection laws require organizations to continuously monitor, update, and enforce their security practices.
Platforms like Salesforce Health Cloud are built with compliance at their core, offering enterprise-grade security features that align with global standards. This allows healthcare providers to innovate without exposing themselves to unnecessary risk.
Building Trust Through Transparency
At the heart of healthcare lies trust.
Patients share their most personal information with the expectation that it will be handled responsibly. Any breach of that trust can have lasting consequences.
Trust is built through:
- Clear data governance policies
- Transparent communication with patients
- Consistent adherence to compliance standards
- Demonstrated commitment to security
“Trust is earned in drops and lost in buckets.” — Kevin Plank
In healthcare, this statement carries even greater weight.
Security as an Enabler, Not a Barrier
There is a common misconception that strong security slows down innovation. In reality, it enables it.
When systems are secure:
- Data can be shared confidently across teams
- AI models can operate on reliable, protected datasets
- Patients are more willing to engage digitally
Security does not hinder progress. It makes sustainable progress possible.
The Bigger Picture
As healthcare transitions to proactive, AI-driven models, the importance of security will only grow.
It is no longer just about protecting data.
It is about protecting relationships, outcomes, and the future of care itself.
And in that future, trust will be the most valuable currency of all.
Challenges in Adopting Proactive Care Models
Transformation comes with challenges.
Common barriers:
- Legacy systems
- Resistance to change
- Data migration complexities
- Skill gaps
Overcoming these requires strategy and expertise.
How to Successfully Transition from Reactive to Proactive Care
A structured approach is essential.
Steps include:
- Consolidate data sources
- Implement CRM platforms
- Integrate AI capabilities
- Train teams
- Optimize workflows
Transformation is a journey, not a switch.
Real-World Use Cases of AI + CRM in Healthcare
Healthcare organizations are already leveraging these technologies.
Use cases:
- Chronic disease management
- Remote patient monitoring
- Automated patient engagement
Example:
A hospital network improved patient engagement by 40% using CRM-driven communication workflows.
The Future of Healthcare: Autonomous, Intelligent, Predictive
Healthcare is steadily moving toward autonomy. Not in the sense of replacing human expertise, but in augmenting it with systems that can think, learn, and act alongside clinicians.
The next phase of healthcare is not just digital. It is intelligent.
As AI and CRM platforms mature—particularly with ecosystems like Salesforce Health Cloud—healthcare systems are evolving from passive tools into active participants in care delivery.
They do not just support decisions anymore.
They drive them.
What Autonomous Healthcare Systems Will Do
- Predict health risks before they surface
By continuously analyzing patient data—clinical, behavioral, and real-time inputs—systems will identify potential health issues long before symptoms appear. Risk becomes visible early, not retrospectively. - Recommend precise interventions
AI-driven engines, powered by tools like Salesforce Einstein, will suggest next-best actions tailored to each patient’s condition, history, and risk profile. Decision-making becomes faster, more consistent, and more accurate. - Automate workflows across the care journey
Routine processes—appointments, follow-ups, care coordination, alerts—will be executed automatically. This reduces administrative burden and ensures no critical step is missed.
From Assistance to Orchestration
Today, technology assists healthcare providers. Tomorrow, it will orchestrate the entire care ecosystem.
- Alerts will not just notify—they will trigger actions
- Insights will not just inform—they will initiate workflows
- Systems will not just store data—they will continuously learn from it
This is the shift from support systems to intelligent ecosystems.
A Glimpse Into the Near Future
Imagine a patient with a history of cardiac issues:
- Wearable devices detect subtle irregularities
- The system flags a potential risk
- A care coordinator is automatically notified
- A follow-up appointment is scheduled instantly
- The patient receives personalized guidance in real time
No delay. No manual intervention. No missed signals.
This is not futuristic speculation. It is already beginning to happen.
The Role of Human Expertise
Autonomy in healthcare does not eliminate the need for clinicians. It elevates their role.
Doctors and care providers will:
- Focus on complex decision-making
- Deliver empathetic, human-centered care
- Interpret and validate AI-driven insights
Technology handles the repetitive and predictive. Humans handle the nuanced and critical.
The Core Shift: From Reactive to Anticipatory
At its essence, this transformation is about mindset.
- From reacting to illness → to anticipating it
- From treating symptoms → to preventing conditions
- From episodic care → to continuous engagement
“The future depends on what we do in the present.” — Mahatma Gandhi
Healthcare is acting on that future now.
The Bottom Line
The future of healthcare is not reactive.
It is not even just proactive.
It is anticipatory.
A system where risks are predicted, actions are recommended, and workflows are executed—before problems ever escalate.
And for organizations that embrace this shift early, the advantage will not just be operational.
It will be transformational.
Why Healthcare Organizations Must Act Now
The shift is already happening.
Organizations that delay risk:
- Falling behind competitors
- Losing patient trust
- Increasing operational inefficiencies

Early adopters gain a significant advantage.
Conclusion: The New Standard of Care
Healthcare is being redefined.
From reactive to proactive. From fragmented to unified. From manual to intelligent.
This is the new standard.
How CloudVandana Enables Proactive Healthcare Transformation
CloudVandana helps healthcare organizations navigate this transformation with precision, clarity, and measurable impact. In a landscape where technology alone is not enough, the focus is firmly placed on outcomes—clinical, operational, and experiential.
The shift from reactive to proactive care requires more than tools. It requires a well-orchestrated strategy, deep platform expertise, and the ability to translate technology into real-world healthcare value.
That is where CloudVandana delivers.
By leveraging platforms like Salesforce Health Cloud and embedding intelligence through Salesforce Einstein, healthcare organizations are empowered to move beyond fragmented systems and adopt a unified, intelligent care model.
From Implementation to Transformation
Many organizations implement technology. Few truly transform with it.
CloudVandana bridges that gap by ensuring that every solution is aligned with:
- Patient-centric care delivery
- Operational efficiency
- Scalable and future-ready architecture
This is not about deploying features. It is about enabling outcomes.
What CloudVandana Delivers
- End-to-end Salesforce implementation
From initial discovery and architecture design to deployment and optimization, every stage is handled with precision. Systems are built to integrate seamlessly into existing healthcare environments. - AI-driven healthcare solutions
Intelligence is embedded at the core. Predictive analytics, risk scoring, and automated insights enable providers to anticipate patient needs and act proactively. - Workflow automation and optimization
Manual processes are replaced with intelligent workflows—automating follow-ups, care coordination, and patient engagement. This reduces administrative overhead and improves consistency. - Data unification and integration
Disparate systems are connected into a single, cohesive ecosystem. Patient data becomes accessible, actionable, and continuously updated—forming the foundation of proactive care.
A Strategic Advantage, Not Just a Technology Upgrade
Organizations that partner with CloudVandana do not just modernize their systems. They redefine how care is delivered.
- Decisions become data-driven
- Engagement becomes continuous
- Care becomes predictive
- Operations become efficient
“Technology delivers value only when it is aligned with purpose.”
CloudVandana ensures that alignment at every step.
The Result: Intelligent Healthcare Ecosystems
With the right strategy and the right implementation, healthcare systems evolve into intelligent ecosystems—capable of:
- Predicting patient risks
- Personalizing care journeys
- Automating critical workflows
- Delivering consistent, high-quality outcomes
This is the foundation of proactive healthcare.
👉 Visit: https://cloudvandana.com
👉 Book your consultation today and lead the future of healthcare.
Frequently Asked Questions (FAQs)
1. What is proactive healthcare?
Proactive healthcare is a care model focused on preventing illness rather than treating it after it occurs. It uses data, AI, and continuous monitoring to identify risks early and enable timely interventions.
2. How is proactive care different from reactive care?
Reactive care responds to symptoms after they appear, while proactive care anticipates health risks before they become critical. The shift is from treatment → prevention, and from episodic care → continuous care.
3. What role does AI play in proactive healthcare?
AI analyzes large volumes of patient data to identify patterns, predict risks, and recommend actions. Tools like Salesforce Einstein help healthcare providers make faster, more accurate decisions.
4. How does CRM help in healthcare transformation?
CRM platforms unify patient data, track interactions, and enable personalized engagement. Solutions like Salesforce Health Cloud create a 360-degree patient view, improving care coordination and decision-making.
5. What is Salesforce Health Cloud used for?
Salesforce Health Cloud is used to manage patient data, coordinate care, automate workflows, and provide real-time insights. It helps healthcare providers deliver personalized and proactive care.
6. Can proactive healthcare reduce hospital readmissions?
Yes. By identifying high-risk patients early and ensuring continuous monitoring and follow-ups, proactive systems can significantly reduce readmissions and improve recovery outcomes.
7. How does predictive analytics improve patient outcomes?
Predictive analytics uses historical and real-time data to forecast potential health risks. This allows providers to intervene early, reducing complications and improving overall patient outcomes.
8. Is proactive healthcare only for large hospitals?
No. Proactive care models can be implemented by hospitals, clinics, and even smaller healthcare providers. Scalable platforms like Salesforce make it accessible for organizations of all sizes.
9. How secure is patient data in AI-driven healthcare systems?
Modern platforms follow strict security protocols, including data encryption, access controls, and audit trails. Compliance with regulations like HIPAA ensures that patient data remains secure and protected.
10. What challenges do organizations face when adopting proactive care?
Common challenges include legacy systems, data silos, resistance to change, and integration complexity. A structured implementation strategy helps overcome these barriers.
11. How long does it take to implement Salesforce Health Cloud?
Implementation timelines vary depending on the complexity of the organization, data migration needs, and integrations. With the right partner, deployment can be streamlined and efficient.
12. How can CloudVandana help healthcare organizations?
CloudVandana provides end-to-end implementation of Salesforce Health Cloud, integrates AI capabilities, automates workflows, and unifies data—helping healthcare organizations transition from reactive systems to proactive, intelligent care models.
By integrating Slack with their CRM and defining structured workflows.

Atul Gupta is CloudVandana’s founder and an 8X Salesforce Certified Professional who works with globally situated businesses to create Custom Salesforce Solutions.
Atul Gupta, a dynamic leader, directs CloudVandana’s Implementation Team, Analytics, and IT functions, ensuring seamless operations and innovative solutions.















